How to Cure a Frozen Shoulder Quickly

 To cure a frozen shoulder quickly, first, it is important to understand the condition, how it changes over time, and what treatments work best at each stage of its development. In most cases, it is a self-limiting condition that resolves completely in between 1- 4 years, but its impact can be lessened and its progress sped up by choosing the right treatments at the right time (1).
To cure a frozen shoulder quickly, first, it is important to understand the condition, how it changes over time, and what treatments work best at each stage of its development. In most cases, it is a self-limiting condition that resolves completely in between 1- 4 years, but its impact can be lessened and its progress sped up by choosing the right treatments at the right time (1).
What is a frozen shoulder?
Frozen shoulder is the descriptive name given to the chronic inflammatory condition Adhesive Capsulitis, a chronic stiffening and painful loss of movement at the glenohumeral joint (the joint that produces most of the shoulder’s movement). The condition is characterized by inflammation and thickening (fibrosis) of the shoulder joint’s capsule leading to pain and very limited movement in the shoulder. There are two types of adhesive capsulitis;
Primary – This is where there is no real reason for it to occur.
Secondary – This is where there was an event that triggered a change in the shoulder’s tissues, often it can occur after shoulder surgery, an injury to the shoulder, or even after a person has a stroke. These events change how the body’s nervous system influences the shoulder by reducing its movement and stiffening the joint (2). Other medical conditions are also associated with adhesive capsulitis, such as diabetes, heart disease, and Parkinson’s disease (3).
Who is more likely to get a frozen shoulder?
Frozen shoulders occur most commonly between the ages of 35-65, 70% of cases are found in women, and diabetics have a 20% chance of suffering from this condition compared to 2-5% of the general population (4). The factors that would make a person develop a frozen shoulder are both genetic and from events that happen to them throughout their life (5).
How to tell if you have got a frozen shoulder?
Often a frozen shoulder is difficult to spot in the early stages as it can appear as if you have a muscle strain, or a stiff neck and shoulder, however, a frozen shoulder has a few defining characteristics that would let you know that you may have one.
1 – There is severe stiffness at the shoulder joint that persists and gets worse over time.
2 – There is quite severe pain, even when you are not using the shoulder and when lying on it while trying to sleep.
3 – There is a nearly full loss of external rotation at the shoulder (turning the shoulder out) when either you try to move it yourself, or another person tries to move it (if it was a muscle strain it would be movable by another person with little pain).
Commonly daily tasks such as putting a jacket on, fastening a bra, or brushing hair will be painful and difficult to do and there may be neck pain due to the muscles around the shoulder try to compensate (1, 6).
An assessment by a medical professional such as an osteopath is advised to ensure you get the correct diagnosis. Once diagnosed, identifying which stage of a frozen shoulder’s course you are in will allow you to put in place a plan to help reduce its impact and shorten its duration (1).
 The Three Stages of Frozen Shoulder
The Three Stages of Frozen Shoulder
Painful freezing phase – Duration 10-36 weeks. Pain and stiffness around the shoulder with no history of injury. A nagging constant pain is worse at night, with little response to non-steroidal anti-inflammatory drugs
Adhesive phase – Occurs at 4-12 months. The pain gradually subsides but the stiffness remains. Pain is apparent only at the extremes of movement. Gross reduction of shoulder movements, with near-total loss of external rotation
Resolution phase – Takes 12-42 months. Follows the adhesive phase with spontaneous improvement in the range of movement. The mean duration from onset of frozen shoulder to the greatest resolution is over 30 months. (1).
Which Treatments Work For a Frozen Shoulder?
Different treatments work at different times throughout the natural course of a frozen shoulder. The first thing that you must do is plan for the journey that the condition will take you on and be prepared to adjust your lifestyle accordingly. Learning about the condition from an experienced medical professional can help greatly in identifying strategies that will speed up your recovery (1).
For most people engaging in a course of physical therapy, combined with home exercise will be the key to a speedy recovery (1, 6), but different strategies are needed for different phases of the condition.
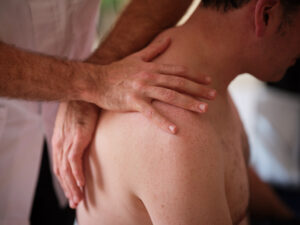
Painful Freezing Stage – THE MAIN OBJECTIVE IN THIS PHASE IS TO REDUCE THE PAIN so it has as little impact on your wellbeing as possible. This is important as the pain is likely to reduce sleep quality which in turn can affect your mood, and your experience of the pain (7). If you do have trouble sleeping, lying on the unaffected side, or your back, while cushioning the arm can help (image). Ice or heat packs may also help in this stage.
In the early phases, a corticosteroid injection has been found to be useful in significantly reducing the pain and limiting the development of fibrosis in the shoulder which would potentially shorten the course of the condition. The earlier the injection is given the better the outcomes, in the short term they can be up to 80% effective in reducing pain and improving function (7), however, the effect is not well maintained throughout the course of the condition and they are best combined with a course of exercise and manual therapy (8).
With exercises and manual therapy, the key takeaway here is in this phase any exercises you perform, or techniques that are applied to the shoulder by a therapist such as an osteopath are PAIN-FREE. People who exercised and had their shoulder mobilised with a pain-free range for 2-5 seconds in this phase showed better outcomes than those who performed painful intensive techniques (1). An experienced therapist such as an osteopath would be able to help you construct a home exercise plan and perform specific techniques to help control the pain in this phase.
 Adhesive Stage – In this less painful stage, the focus should be on increasing the range of movement in the shoulder joint and the surrounding structures of the neck, chest, and shoulder blade, so an osteopath may use more intensive stretching techniques that focus on the restrictions at the limit of the restricted movements and give more wide-ranging stretches for you to do at home (9). The exercises and techniques performed in this phase should be held for a more sustained time (7). Also beneficial in this phase are basic strengthening exercises known as isometric exercises (they are performed with very little movement to avoid provocation of the pain) that will help strengthen the weakened muscles around the shoulder and upper back (9).
Adhesive Stage – In this less painful stage, the focus should be on increasing the range of movement in the shoulder joint and the surrounding structures of the neck, chest, and shoulder blade, so an osteopath may use more intensive stretching techniques that focus on the restrictions at the limit of the restricted movements and give more wide-ranging stretches for you to do at home (9). The exercises and techniques performed in this phase should be held for a more sustained time (7). Also beneficial in this phase are basic strengthening exercises known as isometric exercises (they are performed with very little movement to avoid provocation of the pain) that will help strengthen the weakened muscles around the shoulder and upper back (9).
Resolution phase – This phase is where exercise and manual therapy has the most impact. As the shoulder movement begins to return the process can be significantly affected by introducing more prolonged and aggressive stretches and manual techniques from an osteopath. As soon as the shoulder allows them to be done without pain progressive strength exercises should be prescribed, moving from basic work with bands into more traditional weights and more general shoulder and upper body exercises (9).
What if it doesn’t get better?
There are several other interventions possible if the resolution of the problem is not as predicted, these include more intense interventions such as manipulation under anesthesia to help break down the restrictions or surgical release of the affected tissues. These are usually techniques of last resort, they are usually very successful but carry significant risks (10).
HOW CAN ALIGN BODY CLINIC HELP?

As highly trained experts in the musculoskeletal system, our expert osteopaths can provide you with a thorough assessment and diagnosis of your shoulder, as well as information about the condition, and advice on what to do to help while considering your individual needs. Our hands-on treatments such as stretching and gentle movements of your shoulder and surrounding structures can help ease pain and improve function, and we will also provide individualised home exercise plans to help you get you back to your best as soon as possible.
Do you want to know what is causing your pain and if we can help? Why not take advantage of our new patient assessment introductory offer to get you started towards a tailor-made recovery plan for only £19.
Are you in a lot of pain and want to get better as soon as possible? If so then why not book in for our new patient consultation, with treatment on the day, for £75.
References
1 – Dias R, Cutts S, Massoud S., (2005). Frozen shoulder. BMJ, 331:1453-6
2 – Walmsley S, Rivett DA, Osmotherly PG., (2009). Adhesive capsulitis: Establishing consensus on clinical identifiers for stage 1 using the delphi technique. Phys Ther, ;89:906-917.
3 – Kelley M, Mcclure P, Leggin B., (2009). Frozen shoulder: Evidence and a proposed model guiding rehabilitation. J Orthop Sports Phys Ther, 39:135-148.
4 – Vermeulen HM, Rozing PM, Obermann WR, Cessie S, Vlieland T., (2006). Comparison of high-grade and low-grade mobilization techniques in the management of adhesive capsulitis of the shoulder: Randomized clinical trial. Phys Ther,86:355-368.
5 – Hakim AJ, Cherkas LF, Spector TD, MacGregor AJ., (2003). Genetic associations between frozen shoulder and tennis elbow: a female twin study. Rheumatology (Oxford), 42:739-742.
6 – Mezian K, Chang KV. Frozen Shoulder. InStatPearls [Internet] 2019 Feb 25. StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482162/. In – https://www.physio-pedia.com/Adhesive_Capsulitis#ppm43951, accessed 3/8/2021.
7 – Brue S et al., (2007) Idiopathic adhesive capsulitis of the shoulder: a review. Knee Surg Sports Traumatol Arthrosc. 15:1048-1054.
8 – Blanchard V, Barr S, Cerisola FL., (2010) The effectiveness of corticosteroid injections compared with physiotherapeutic interventions for adhesive capsulitis: A systematic review. Physiotherapy, 96: 95-107.
9 – Chan, H., Pua, P. Y., & How, C. H. (2017). Physical therapy in the management of frozen shoulder. Singapore medical journal, 58(12), 685–689.
10 – Hamdan TA, Al-Essa KA., (2003) Manipulation under anaesthesia for frozen shoulder. Int Orthop, :27: 107-9.


 The Three Stages of Frozen Shoulder
The Three Stages of Frozen Shoulder